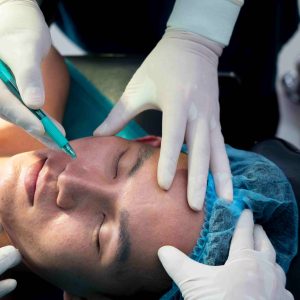
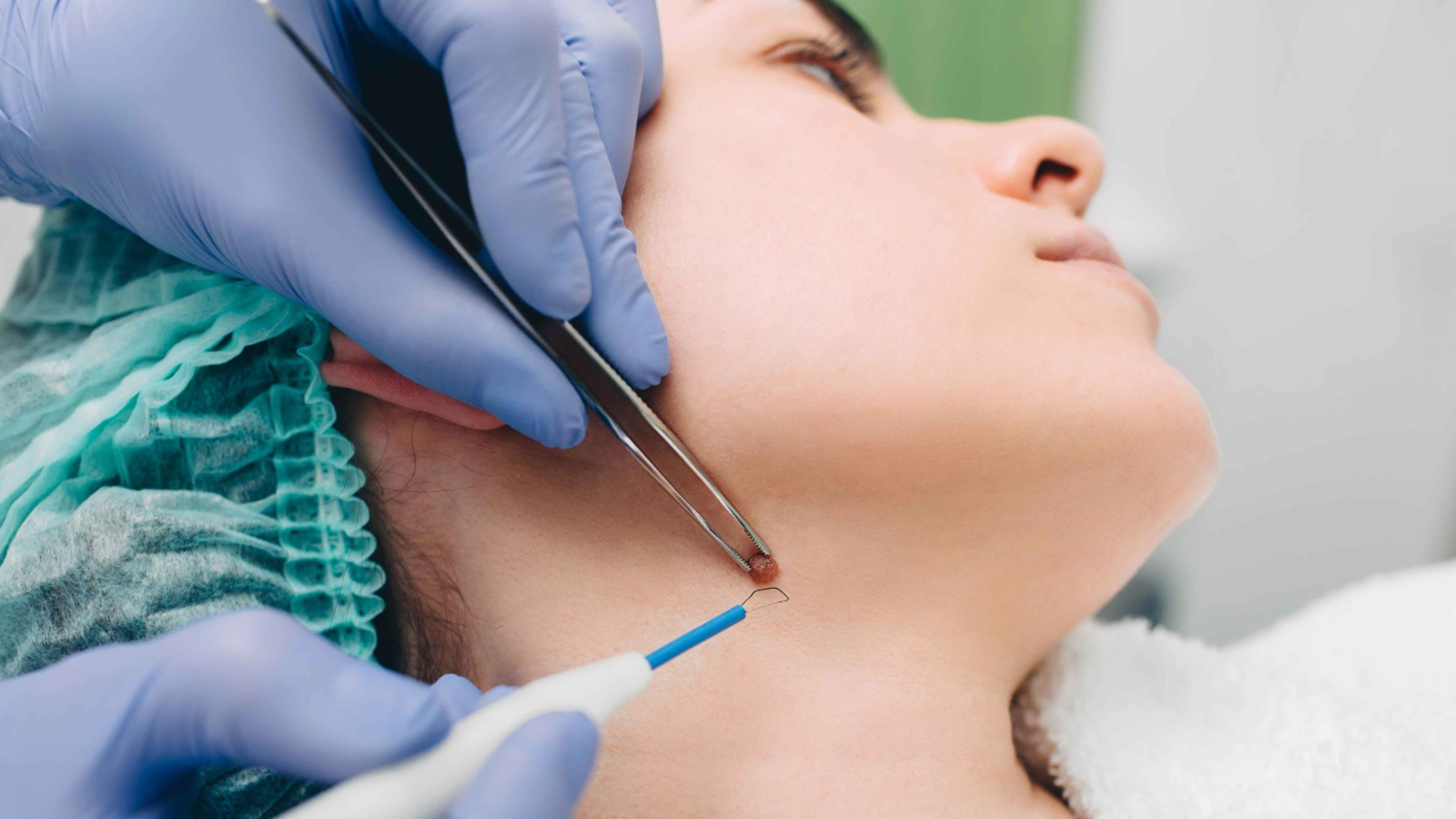
About 3% of adults between the ages of 20 and 60 have hyperhidrosis, a disorder causing too much sweating outside of normal body temperature control. Though good management techniques exist, this illness can seriously affect quality of life.
What is Hyperhidrosis?
Eccrine glands overworking themselves to generate more sweat than required for cooling causes hyperhidrosis. This excessive sweating occurs sporadically without apparent triggers, at rest, in cold conditions, or otherwise.
Types of Hyperhidrosis
Primary Focal Hyperhidrosis
- Genetic disorder passed on from the biological family
- influences particular areas: hands, feet, underarms, face
- Usually starts before one reaches 25.
- Most typically occurring kind
Secondary Generalized Hyperhidrosis
- Underlying medical diseases cause generalised
- Side effects of some drugs
- It might bring nighttime sweating.
- influences the whole body
Common Causes of Hyperhidrosis
Medical Conditions
- Hypertensive thyroidism
- Diabetes, Heart disease
- Parkinson’s disease
- Manopause
- Anxiety disorders
Medications That Trigger Sweating
- Sertraline, bupropion; antidepressants
- Painkillers, such as hydrocodone
- Lisinopril, a blood pressure reliever
- Thyroid drugs, often known as levothyroxine
- Naproxen, an anti-inflammatory medication
Environmental Triggers
- Anxiety and tension
- Moderate temps
- Physical exercise
- Foods with spices or fat
- Strong drinks with caffeine
- Drink alcohol.
Symptoms and Affected Areas
Usually affecting areas rich in eccrine glands, hyperhidrosis:
Most Common Locations
- Mostly prevalent, palmar hyperhidrosis is sweaty palms.
- Underarm sweating from axillary hyperhidrosis
- Plantar hyperhidrosis—sweaty feet
- Face and forehead sweating in craniofacial hyperhidrosis
Associated Symptoms
- Skin and clothes are wet
- Sweat beads on the face
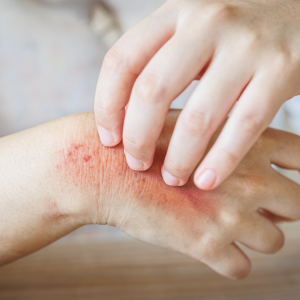
- Skin irritation and inflammation
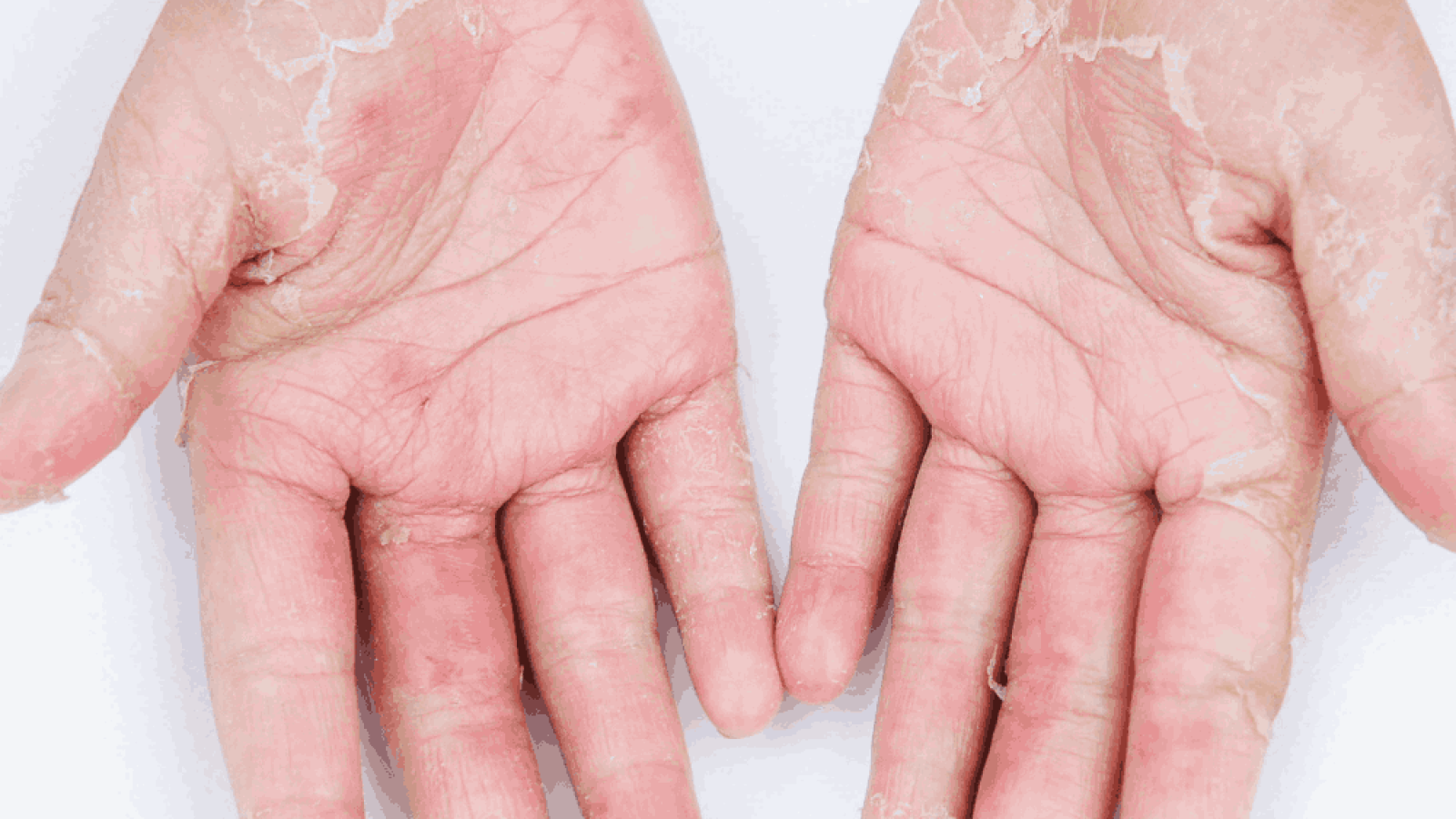
- Broken or peeling skin on the feet
- Body smell resulting from bacterial multiplication
Diagnosis Methods
Medical professionals apply particular diagnostic guidelines. A hyperhidrosis diagnosis calls for at least six months of excessive sweating plus two of these elements:
- Underarms, palms, soles, or the face—sweating happens here.
- Two sides of symmetric sweating
- Either little or no night sweating
- Weekly episodes of sweating
- Ancestral hyperhidrosis history
- Interference with daily responsibilities
- Less than 25 years of age
Diagnostic Tests
- Test with starch-iodine: The Solution gets dark blue in places of increased perspiration.
- Test for papers: Special paper scales the generation of sweat.
- Blood tests: Rule out fundamental diseases.
- Thermoregulatory test for sweat: Analyzes perspiration trends.
Treatment Options
Lifestyle Management
At-Home Strategies
- Use antiperspirants with aluminium bases (6–20% aluminium chloride).
- Before sleeping, treat dry skin.
- Select natural, breathable materials such as cotton, wool, and silk.
- Take more showers.
- Change socks one to two times a day.
- During exercise, use moisture-wicking fabrics.
Footwear Tips
- Choose leather shoes with air flow.
- Get shoe insoles and foot powder.
- Wherever feasible, wear sandals.
- Select pantyhose with cotton soles.
Medical Treatments
Prescription Medications
- Stronger formulations of aluminum chloride antiperspirants
- Glycopyrrolate and oxybutynin are anticholinergic drugs.
- Glycopyrrolate prescription creams
- Medicated wipes based on glycopyrronium tosylate
- Treatments for anxiety-related sweating using antidepressants
- Beta-blockers for handling triggers
Advanced Therapies
- An injection of botulinum toxin blocks nerve signals to sweat glands; results last six months.
- Low electrical current stops sweat glands in 10 to 20 minute sessions.
- Microwave therapy: permanently damages sweat glands by thermal energy
Surgical Options
Minimally Invasive Procedures
- Endoscopic thoracic sympathectomy (ETS) slices nerves regulating sweat output.
- The removal of sweat glands: Applications include laser procedures, liposuction, or curettage.
- Sympathotomy: Interferes with nerve signals without cutting any nerves
Surgery is reserved for extreme instances refractory to other therapies because of possible consequences, including compensatory sweating.
Prevention and Management Tips
Preventing Flare-ups
- Control underlying medical disorders
- Steer clear of known triggers—spicy foods, coffee.
- Implement strategies for stress reduction.
- Practice good hygiene.
- Keep drinking.
Long-term Management
- Work with medical professionals for changes in medications.
- Think about alternative treatments, including combinations.
- Keep an eye on skin problems.
- Talk on the effects on mental health.
Mental Health Considerations
Extreme emotional discomfort brought on by hyperhidrosis might lead to social disengagement and activity avoidance. Many people are ashamed of obvious sweating or worry about the responses of others.
Expert advice helps control emotional effects as well as physical ones. Mental health experts can offer ways for confidence-building and coping mechanisms.
Conclusion:
Hyperhidrosis Treatment depends on knowing your particular kind, triggers, and treatment reaction. Dealing with seasoned medical professionals guarantees correct diagnosis and treatment preparation.
See a licensed dermatologist at Cleo Clinical Care for a professional assessment and tailored treatment recommendations. If you’re searching for a dermatologist near me, our clinic provides expert care with proven results.
Furthermore, supporting general treatment effectiveness is maintaining good skin health with suitable skincare products from The Skin Theory.
FAQ’s:
Is a total cure from hyperhidrosis possible?
Although there is no cure for primary focal hyperhidrosis, therapies help to greatly control symptoms. Once the underlying reasons are addressed, secondary hyperhidrosis may go away.
At what age does hyperhidrosis usually first strike?
While secondary hyperhidrosis can strike at any age depending on underlying factors, primary hyperhidrosis usually starts before age 25.
Is inherited hyperhidrosis?
Indeed, because of genetic abnormalities influencing sweat gland function, primary focal hyperhidrosis typically runs in families.
For what duration do therapy results hold?
Antiperspirants work daily; Botox lasts six months; iontophoresis calls for maintenance visits; and surgery yields permanent benefits. Treatment times vary.
For what reason should I consult a doctor regarding too much sweating?
See doctors when sweating interferes with everyday activities, causes emotional discomfort, or develops with nausea, dizziness, or chest pain.