Mycoses, fungal infections, occur when dangerous fungi attack the body and overpower the immune system. Millions of people worldwide suffer from these infections; they might strike internal organs, skin, nails, or hair. This thorough book addresses all you need to know about fungal infections, their symptoms, causes, and the most successful Fungal Treatments.
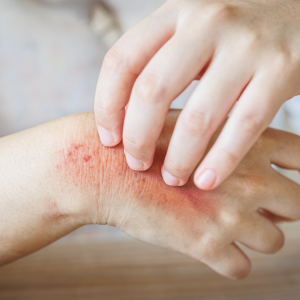
What Are Fungal Infections?
Fungal infections are diseases brought on by fungi, yeasts, or molds that attack and proliferate in several body areas. Although many fungi dwell on our bodies naturally without causing any issues, several diseases can induce overgrowth and illness.Types of Common Fungal Infections
Ringworm (Tinea Corporis)
On the skin, ringworm shows as round, itchy lesions with elevated margins. Though its name suggests otherwise, fungus rather than worms causes it. The infection might show up:- Pink or crimson tones on lighter skin
- Grey or brown tones of a darker complexion
- With a centre of clear skin and expanding margins
Athlete’s Foot (Tinea Pedis)
Like shoes, stockings, and locker rooms, this common foot infection thrives in warm, damp surroundings. See for:- Skin breaking or peeling between the toes
- Burning feelings, stinging, or itching
- Blisters and discoloration occasionally
- Layered soft or breaking down skin
Jock Itch (Tinea Cruris)
Particularly in warm, humid environment, jock itch mostly affects the groin, buttocks, and inner thighs. Among the symptoms are:- Groin region flaky, scaly skin
- Chafing and acute itching
- Ringed circular rash with elevated margins
- Discolouration: gray/brown on darker skin, red or pink on light skin
Yeast Infections (Candidiasis)
Overgrowth of candida can impact many body areas:- Infections involving vaginal yeast: Pain, itching, odd discharge
- White patches in the mouth or throat are oral thrush.
- Diaper rash is red, inflamed skin in the diaper area.
- Nails that are discoloured, thick, or cracked:
Causes of Fungal Infections
- Harmful fungi invade via wounds or cuts to cause fungal infections.
- Natural fungi on your body proliferate in response to environmental factors.
- Your system of immunity gets impaired.
- Antibiotics throw off the microbial natural equilibrium.

Common Fungi Found to Cause Illnesses:
- Dermatosites: Target keratin in nails, skin, and hair.
- Candida: A naturally occurring yeast that can proliferate excessively
- environmental fungus: From water or soil, Histoplasma, Aspergillus
Factors of Risk
If you run a higher risk of fungal diseases.- Have cancer or HIV/AIDS and a compromised immune system.
- Take some drugs, including immunosuppressants and antibiotics.
- Deal with weak circulation or diabetes.
- Spend time in public areas that have been damp, pools, locker rooms.
- Live in tropical, warm environments.
- Wear tight, non-breathable garments.
- Feel as though you sweat excessively.
Diagnosis and Testing
Healthcare professionals identify fungal infections using visual inspection of impacted sites.- Examined under a microscope: skin, nail, or tissue samples
- Cultures to proliferate and name the particular fungus
- Imaging for deep fungal infections or blood testing
Effective Treatments
Topical Treatments
- powders, sprays, and antifungal creams
- Over-the-Counter Fungal Treatments for Minor Illnesses
- Prescription-strength formulas for severe conditions
Oral Medications
- Designed for either severe or recurring infections
- usually required in systemic conditions or nail infections
- could call for weeks or months of therapy.
Home Care
- Maintaining the affected areas dry and clean
- Treat scalp problems using medicated shampoos.
- Change your pants and socks.
- Give the impacted areas breathing room.
Prevention Strategies
With these basic habits, avoid fungal infections:- Keep up decent personal cleanliness.
- After bathing, dry completely, especially between toes.
- Choose cotton, breathable pants, and socks.
- Share personal objects like towels or hairbrushes only.
- In public restrooms and locker rooms, wear sandals.
- Change straight away from moist clothes.
- In warmer conditions, avoid tight-fitting clothing.
- Use powder antifungals in shoes or trouble areas.
When to See a Dermatologist
See a dermatologist if you run across:- Infections that worsen with over-the-counter medication
- Recurrent fungal diseases
- Distributing illness or severe symptoms
- Infections alongside immunological problems or diabetes
- Unusual or extreme discomfort
Fungal Infections and Skincare
Appropriate skincare products from The Skin Theory can help control and avoid fungal infections. Check for:- Non-comedogenic moisturisers
- Products marked “fungal acne safe” use ingredients like ketoconazole or zinc pyrithione.
- pH-based cleaners

Add a Comment