With eczema and psoriasis among the most common yet sometimes misdiagnosed dermatological problems, skin disorders can seriously affect quality of life. Although at first glance many disorders have similar symptoms, their different traits influence diagnosis and treatment.
This thorough guide looks at the important variations between eczema and psoriasis to enable you to better identify their symptoms, understand these disorders, and find suitable treatment.
Visual Appearance: How to Tell Them Apart
Eczema’s Distinctive Look
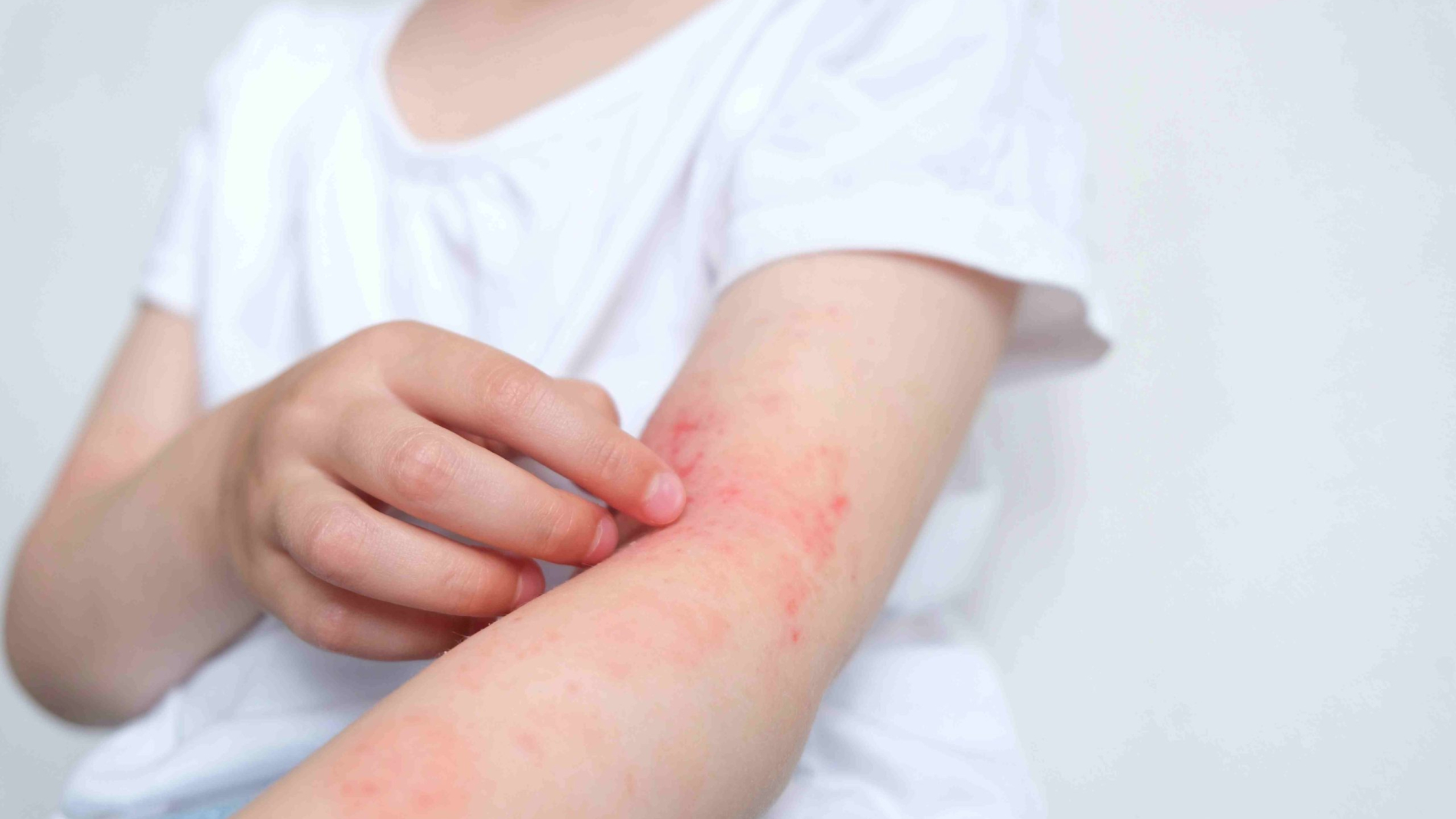
Usually, eczema shows as reddish spots with ill-defined edges. On lighter skin tones, these patches show as pink to red with probable crusting and pimples. Eczema may show up on darker skin tones as little dry bump-filled dark brown, grey, or purple areas.
During severe flares, the affected skin may ooze or leak and appear rough, puffy.
Characteristic Appearance of Psoriasis
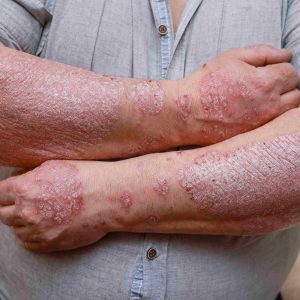
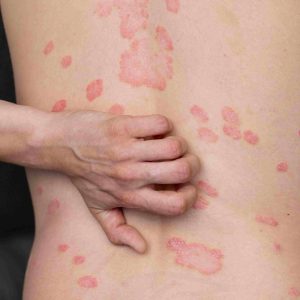
Psoriasis shows itself as well-defined, thick plaques with silvery or white scales. More defined borders than eczema patches, these plaques are elevated. Accelerated skin cell proliferation causes the skin buildup seen in psoriasis to be thicker, with more inflammatory areas that do not mix into the surrounding skin as eczema does.
Location Patterns: Where They Typically Appear
Common Eczema Sites
Usually developing in skin fold areas or “flexor” surfaces, eczema
- In the elbows
- Behind knees
- Front of the neck
- Ankles and wrists
- Particularly in young children, facial areas
- Adult hands
Typical Locations for Psoriasis
Psoriasis has a distinct distribution pattern and usually affects:
- Extensor surfaces, such as the knees’ and elbows’ exterior surfaces
- Scalp and haversine
- Lower back
- Nails (pitting, discoloration)
- ears and behind ears
- Soles and palms, especially in some kinds
Usually, one of the first hints for differentiating between these disorders is the location difference.
Sensation Variations: Itches against Pain
The sensory perception of these disorders is somewhat different:
The severe itching of eczema
The hallmark of eczema is intense itching (pruritus), which can:
- Get strong enough to cause disturbance of sleep.
- Lead to a destructive cycle of scratch-itch.
- worse at night
- cause great misery and lower quality of living.
The Burning Sensation of Psoriasis
Although psoriasis can cause itching, usually it is marked by:
- Burning or stinging experiences
- Mild to moderate itching (less than in eczema)
- Skin stiffness and discomfort, particularly during flares
- More discomfort than strong itching
Immune System Involvement
Both disorders include malfunction of the immune system, albeit via different channels:
Eczema’s Immune Reaction
Eczema is the outcome of an excessive immune response, including:
- T-cells of Th2 predominance
- Relation with inflammation of the allergic kind
- Potential hereditary elements influencing the function of skin barriers
- Many patients have filaggrin gene mutations.
The immune system mechanism of psoriasis
Psoriasis results from another immunological mechanism involving:
- Th1 and Th17 T-cell activation
- Generating particular inflammatory cytokines
- speeded-up skin cell turnover—days rather than weeks
- Involvement of the immune system is usually employed in the fight against bacterial and fungal infections
These different immune systems help to explain why medications aiming at particular pathways benefit one ailment but not the other.
Age of Beginning and Demographics
Furthermore, unique characteristics of these disorders are their frequency and timing, which provide:
Eczema Patterns
- Affect roughly thirty million Americans
- Usually starts in childhood, often before age five.
- With ageing, it may either improve or resolve
- Common in homes where allergies or asthma run in the family
Psoriasis
- Affects around 8 million Americans.
- usually shows up after age 18.
- often lasts all of life.
- May exhibit family trends devoid of significant allergic links.
Sets off and influences Flare Factors
Knowing the reason for flares will assist one in controlling their condition:
Often used Eczema Set off
- environmental allergies (pet dander, dust mites)
- Sensitivities or food allergies
- Strong cleansers, detergents, and perfumes
- Some fabrics (particularly synthetic fibres and wool)
- Anxiety and stress
- Changing weather and sweating
- Hormonal swings
Typical Psoriasis: Causes
- Trauma or skin injuries ( Koebner phenomenon)
- Diseases, especially streptococcal
- Some drugs, including lithium and beta-blockers,
- dry, frigid conditions
- Alcohol intake
- Stress from Smoking
- Sunburn Remedial Strategies
Treatment Approaches
While some treatments cross over, many are condition-specific:
Eczema Treatment Choices
- Frequent emollient-based moisturising
- Topical corticosteroids to reduce inflammation
- Calcineurin inhibitors (TCIs) topically
- Antihistamines are used in the treatment of itching
- Biologics aiming at particular immunological channels (such as dupilumab)
- JAK inhibitors in more severe instances
- Therapy with wet wraps
- Taking care of allergies and triggers
Treatment Approaches for Psoriasis
- Topical treatments—corticosteroids, vitamin D analogues)
- Phototherapy (UVB or PUVA)
- Methotrexate, cyclosporine, or another systemic drug
- Biologics aimed at TNF-alpha, IL-17, IL-23—different from eczema biologics
- Retinal medications orally
- Making coal tar preparations
- Salicylic acid for the reduction of scale
Conditions and Comorbidities
Every illness raises different related health issues:
Eczema. Comorbidity
- Asthma
- Allergy rhinitis
- Food allergies:
- Sleep disturbances brought on by itching
- Higher chance of skin infections
- More sadness and anxiety
Psoriasis Comorbidities
Psoriatic arthritis (affects thirty percent of individuals)
Cardiovascular ailment
Syndrome of metabolic change
Diseases of inflammation in the gut tracts
Increased susceptibility to depression
Possible relationship with other autoimmune diseases
Daily Maintenance and Lifestyle Issues
Beyond medical care, lifestyle changes are quite important:
Living with eczema
- Mild skincare regimens using items free of fragrances
- cotton bedding and clothes
- Dry environment humidifiers
- Develop tactics for trigger avoidance.
- Regular schedule of moisturising
- Methodologies of stress management
- Brief lukewarm showers or baths
Having Psoriasis: Living
- Constant exfoliation helps control scales.
- Moisturising using thicker ointments
- Preventing skin damage wherever is at least possible
- Sun exposure (moderate, measured levels)
- Anti-inflammatory dietary concerns
- Managing weight
- Limit on alcohol
- Quit smoking
When should someone see a dermatologist?
Professional evaluation is indispensable for:
- Correct diagnosis between psoriasis and eczema
- Extreme or pervasive symptoms
- Problems not responding to over-the-counter remedies
- Signs of an infection: yellowish discharge, more discomfort, fever
- Joint pain or swelling—possible psoriatic arthritis
- major influence on emotional or quality of life
Conclusion:
Although at first glance eczema and psoriasis seem identical, their differing appearances, locations, sensations, causes, and treatment techniques make them separate diseases needing different care strategies.
Knowing these variations will enable you to take suitable action towards controlling your skin condition and interact more successfully with medical professionals.
For expert advice, dermatologist-recommended skincare products, and support in managing conditions like vitiligo and eczema, visit Cleo.pk, your trusted resource for skincare products from The Skin Theory and finding a dermatologist near me in Pakistan.
FAQ’s:
1. How is eczema visually different from psoriasis is mostly?
Whereas psoriasis shows thick, scaly plaques with sharp edges, eczema exhibits red, leaking areas with less-defined borders.
2. Where usually do eczema and psoriasis show up?
While psoriasis typically shows on extensor surfaces like the elbows, knees, and scalp, eczema sometimes affects skin folds (elbows, knees).
3. Psoriasis vs eczema: Which condition itches more?
While psoriasis may produce burning or stinging with mild to moderate itching, eczema is usually itchier and more acute.
4. Do psoriasis and eczema have separate causes?
Indeed, allergies and irritants often cause eczema; psoriasis flares with skin damage, infections, or stress.
5. Can one treat psoriasis and eczema the same way?
Not exactly; certain therapies cross, but psoriasis usually calls for separate drugs, particularly biologics aimed at particular immune pathways.

Add a Comment