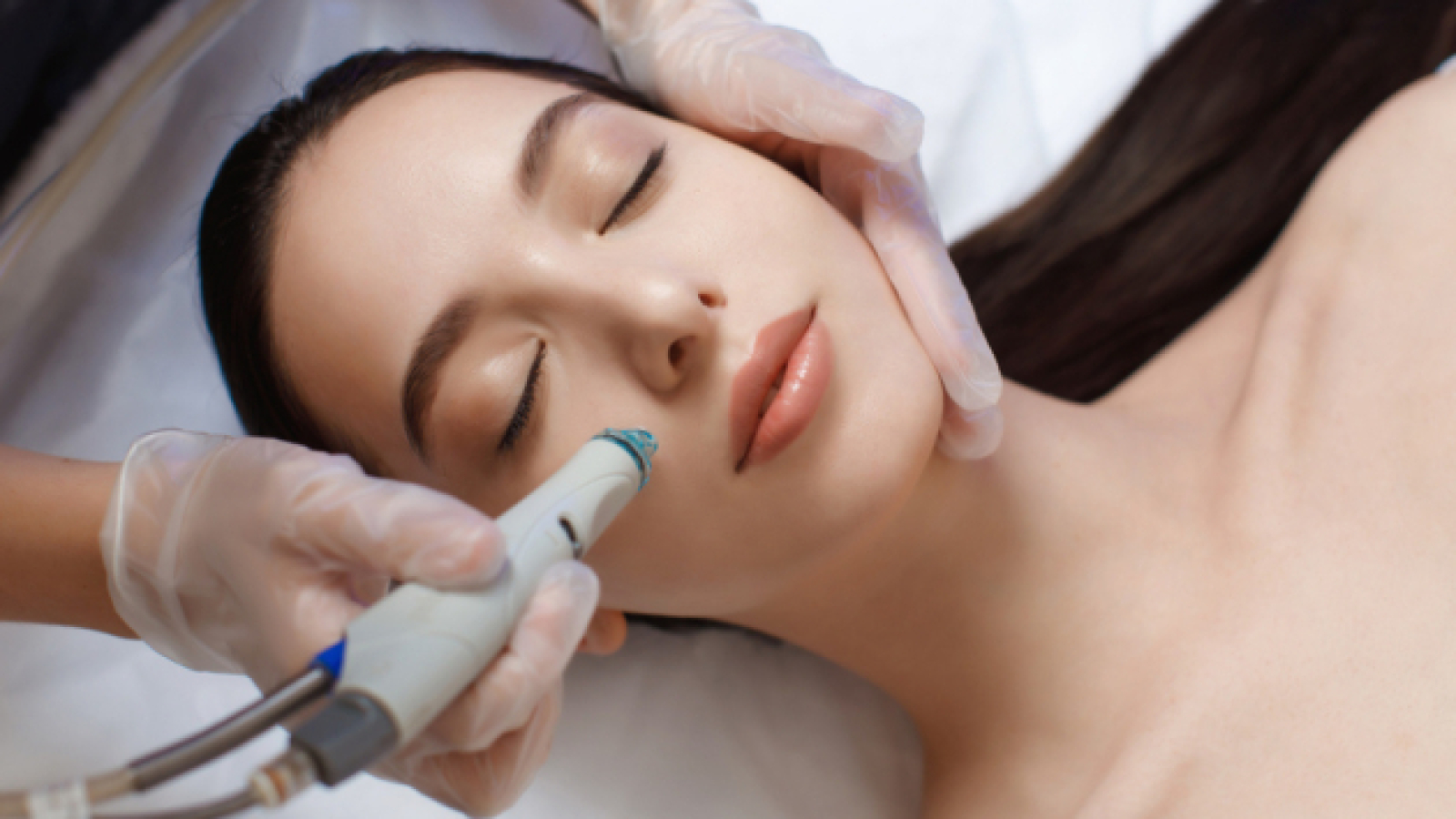
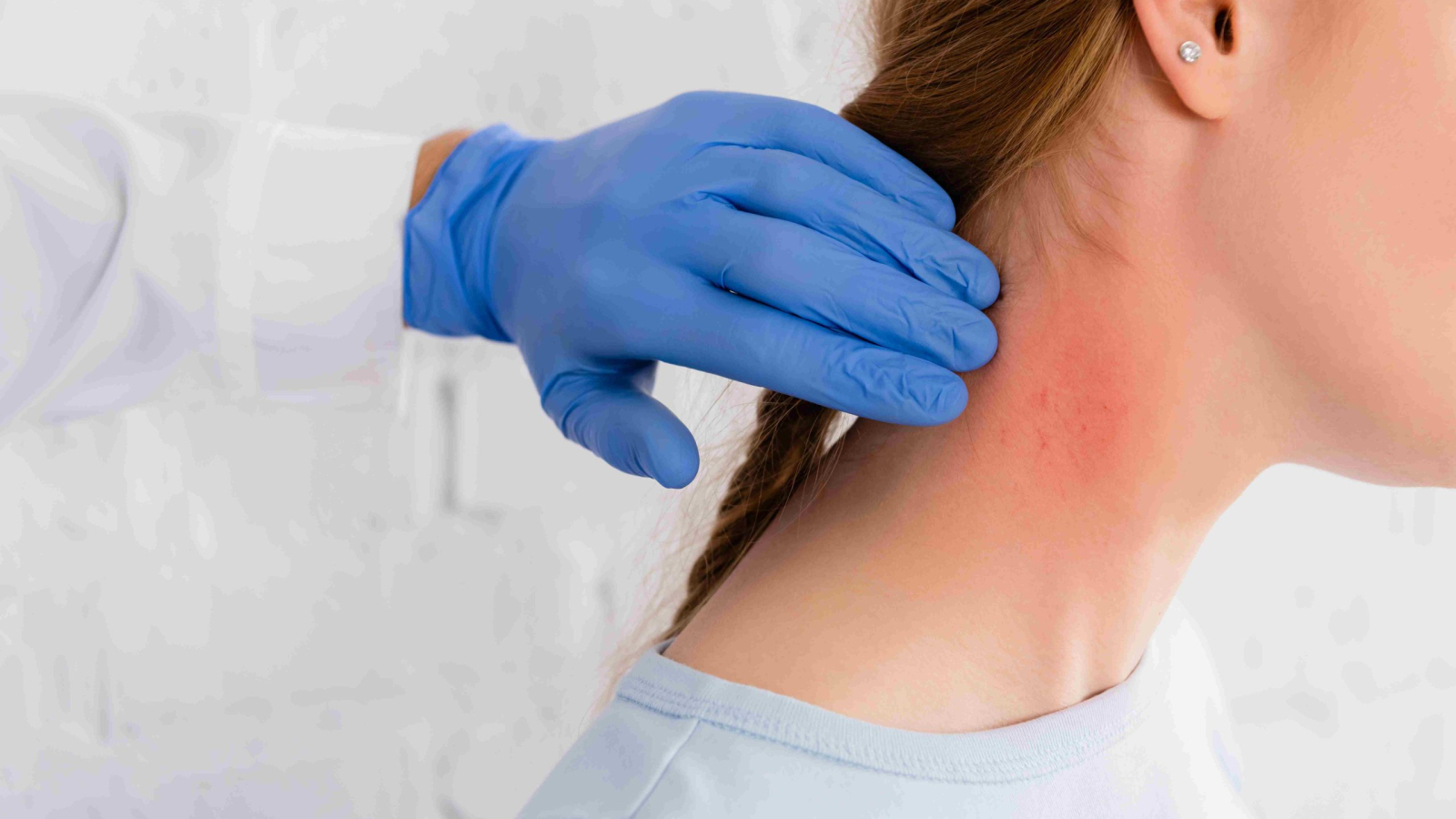
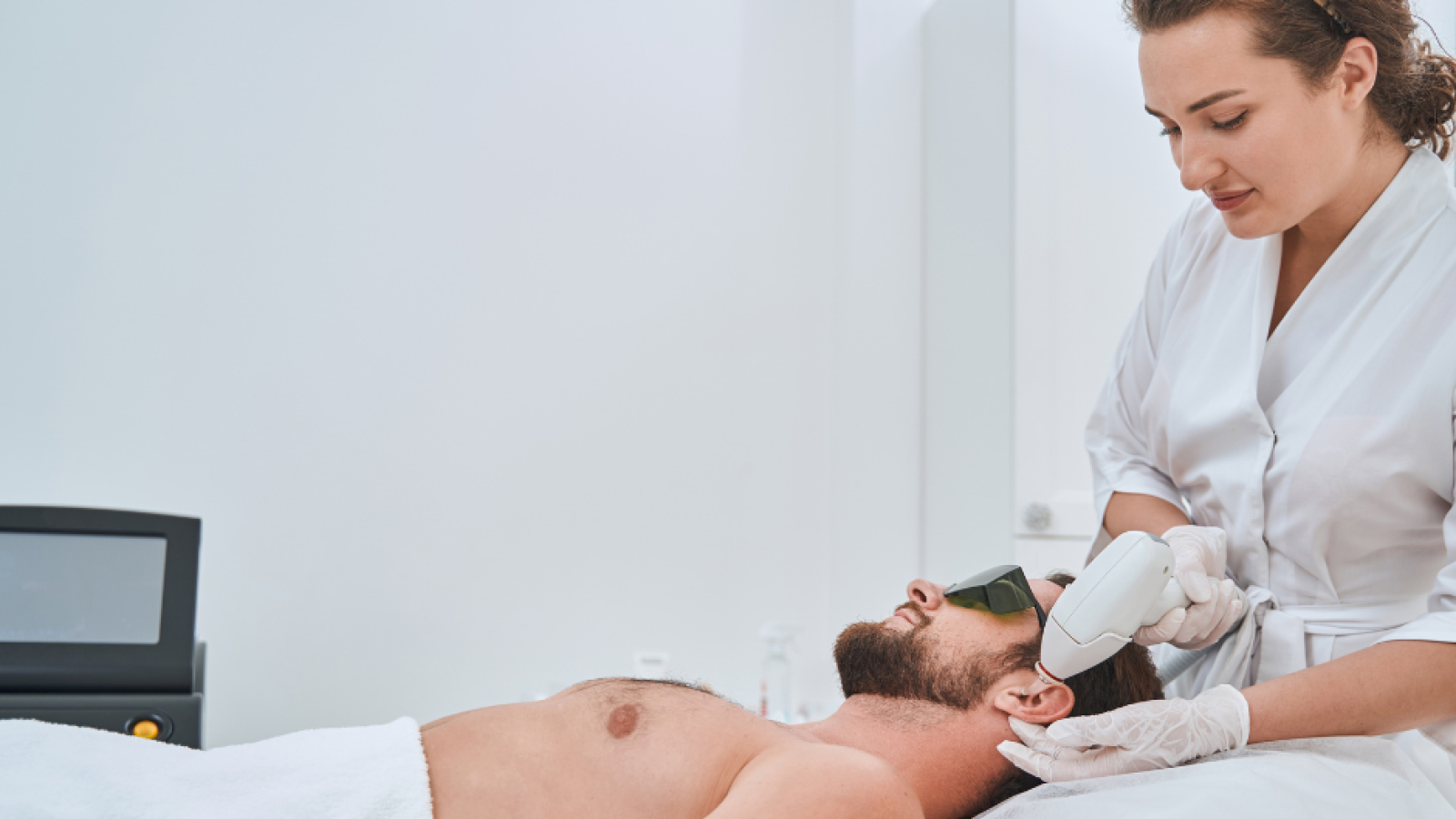
When it comes to eliminating unwanted hair, two highly effective methods stand out: laser hair removal and electrolysis hair removal. Both are designed to reduce or remove hair over the long term, but they each work in unique ways and offer distinct benefits.
Electrolysis Hair Removal: The Permanent Solution
Electrolysis is another popular and effective hair removal method. Electrolysis hair removal uses an electrical current to destroy the hair follicle’s ability to grow hair. A tiny needle is inserted into the follicle, and a small electrical current is applied.
This current disrupts the follicle, preventing future hair from growing. It’s a method that has been used for decades and remains a reliable choice for permanent hair removal.
Electrolysis can be used on almost any part of the body, including delicate areas like the eyebrows, chin, and upper lip.
One of the greatest advantages of electrolysis is its versatility—it works on all skin types and hair colors, making it suitable for nearly everyone. Whether you have fine, coarse, light, or dark hair, electrolysis offers a permanent solution for unwanted hair.
Each electrolysis session can take more time compared to laser hair removal, as it targets individual hair follicles one by one. The process may take longer depending on the area being treated and the density of hair. However, it offers permanent results, meaning once a follicle is treated, it will never grow hair again.
At Cleo, we offer electrolysis as a permanent hair removal option. Our team ensures that the procedure is done with care, targeting each hair follicle with precision to guarantee the best results.
Electrolysis Hair Removal Procedure
The electrolysis procedure begins with a consultation to evaluate the hair growth pattern, skin type, and areas of concern. The skin is then cleansed, and a fine needle is inserted into each hair follicle. The needle releases a small amount of electrical current, which heats the follicle, effectively destroying its ability to grow hair.
Electrolysis is typically more time-consuming than laser hair removal because each follicle is treated individually. The procedure can be done on smaller or larger areas, but the number of follicles to be treated will influence the overall treatment time. For example, a session on the upper lip may take just 15 minutes, while larger areas like the legs could take up to an hour or more.
During the procedure, patients may feel a slight tingling or stinging sensation as the current is applied. Though it is generally well tolerated, some individuals may experience slight discomfort, especially in sensitive areas. Redness or swelling can occur, but it usually disappears after a few hours.
After the treatment, patients are advised to avoid hot showers, direct sunlight, and tight clothing that could irritate the skin. Electrolysis typically requires multiple sessions for optimal results, especially for individuals with dense hair or larger treatment areas.
Benefits of Electrolysis Hair Removal
Electrolysis, known for its long history of effectiveness, offers unique advantages:
- Permanent hair removal: Unlike many other methods, electrolysis offers a permanent solution to unwanted hair. Once a follicle is treated, it will no longer produce hair, making it an ideal choice for those seeking a lifelong solution.
- Versatility: Electrolysis works on all hair types and colors, making it suitable for virtually everyone. It is particularly beneficial for individuals with light hair, which may not respond as well to laser treatments.
- Suitable for small and sensitive areas: Electrolysis is effective for treating small or sensitive areas of the body, such as the eyebrows, upper lip, and chin. It provides precise control, allowing for detailed and targeted treatment in hard-to-reach areas.
- Safe for all skin types: Since electrolysis does not rely on pigmentation, it is safe for use on all skin tones, unlike laser hair removal, which can be less effective on darker skin tones.
- No risk of hyperpigmentation: Electrolysis does not carry the same risk of pigmentation changes as laser hair removal. This makes it a safer option for individuals with darker skin tones.
Each method has its distinct advantages. The choice of electrolysis hair removal or laser hair removal depends on your skin type, hair color, treatment area, and long-term goals.
Electrolysis Hair Removal Cautions
While electrolysis is a safe and effective method, there are some things to consider before undergoing treatment:
- Pain and Discomfort: Electrolysis may cause more discomfort compared to laser hair removal, especially in sensitive areas. The sensation is often described as a mild stinging or tingling. Topical numbing creams may be used to reduce discomfort, but it can vary depending on your pain tolerance.
- Skin Irritation: After the treatment, you may experience slight redness, swelling, or irritation in the treated area. These symptoms are usually temporary and should resolve within a few hours to a few days. However, some individuals may experience longer-lasting skin irritation.
- Multiple Sessions Required: Electrolysis often requires multiple sessions to achieve optimal results. Each treatment focuses on one follicle at a time, which means it may take longer to treat larger areas compared to laser hair removal.
- Risk of Scarring: In rare cases, electrolysis can cause scarring, especially if the needle is inserted too deeply into the skin. This is why it is important to choose a skilled hair specialist who uses proper techniques and equipment.
- Pre-Treatment Care: Like laser hair removal, it’s important to avoid sun exposure before electrolysis treatment. Tanning or sunburned skin may lead to increased sensitivity, which can cause additional discomfort during the procedure.
Electrolysis Hair Removal: Number of Sessions
Electrolysis is a gradual process that involves treating individual hair follicles one at a time. As a result, it often requires more sessions than laser hair removal, especially for larger areas.
- Typical Number of Sessions: The number of sessions needed for electrolysis varies depending on the size of the area and the density of hair. Smaller areas, like the upper lip, may take around 10 to 15 sessions, while larger areas, such as the legs, may require 30 to 40 sessions or more.
- Session Frequency: Electrolysis sessions are typically spaced about 1 to 2 weeks apart to allow the treated follicles to heal and to ensure that new hair growth is addressed. Because electrolysis targets each follicle individually, treatment times can be longer, especially in areas with dense hair.
- Long-Term Results: After a series of treatments, electrolysis offers permanent hair removal. However, it is important to complete all recommended sessions to ensure that all hair follicles are properly treated and that hair regrowth is minimized.
Electrolysis Hair Removal Cost
Electrolysis is another popular method of permanent hair removal, but it generally requires more time and effort, which can influence the cost.
- Factors Affecting Cost: The overall cost will depend on the number of sessions required, the density of hair, and the area being treated. Areas with dense hair growth may require more sessions, which increases the cost. Electrolysis is generally more time-consuming, so longer sessions can lead to higher costs.
- Electrolysis Hair Removal Cost in Pakistan: In Pakistan, electrolysis treatments typically cost around PKR 2,500 to PKR 8,000 per session, depending on the treatment area and the number of follicles being treated. Larger areas or denser hair will require more sessions, leading to higher total costs.
- Permanent Results: Despite the higher upfront cost, electrolysis offers permanent hair removal, making it a cost-effective option in the long term. After completing the necessary sessions, you can enjoy hair-free skin without the need for further treatments.
Finding Hair Removal Services Near You
Finding the right skin care clinic or specialist for your hair removal treatment is crucial to ensuring both safety and effectiveness. Searching for laser hair removal near me can help you identify qualified providers who offer the services you need.
Choosing a Reputable Clinic
When looking for a clinic, it’s important to choose one that uses up-to-date equipment and employs experienced professionals. Make sure the clinic has a reputation for safety and customer satisfaction. Reviews from past clients can be a great way to gauge the quality of service.
Electrolysis Hair Removal Near Me
Electrolysis is a less commonly offered service than laser hair removal, so it’s important to find a clinic with specialists trained in electrolysis. Look for clinics that offer consultations to discuss your hair removal goals and treatment plan.
Factors to Consider
Location, pricing, and equipment are essential factors when selecting a clinic. Ensure that the clinic offers a consultation before treatment, where they can assess your needs, discuss any potential risks, and explain the procedure in detail.
For those in Pakistan, specifically in Lahore, finding quality laser hair removal in Lahore services is important. Look for clinics with good reviews and experienced technicians who understand different skin types and hair concerns.
Hair Specialists & Expertise
When considering hair removal treatments, it’s essential to choose a hair specialist who is experienced and skilled in performing the procedure. Whether you’re opting for electrolysis hair removal or laser treatment, a qualified professional ensures that you receive the best possible treatment while minimizing the risks.
Experienced Professionals
A trained specialist can evaluate your skin type, hair color, and any medical conditions that may affect your treatment. At Cleo, Dr. Amna’s expertise ensures that each patient receives personalized care. The right specialist will assess the best approach for your unique needs, helping you achieve the best results.
Importance of Expertise
An experienced professional can reduce the risk of complications, such as burns, scarring, or pigmentation changes. They are also able to adjust the settings of the treatment based on your skin’s sensitivity and hair type to maximize the effectiveness of the procedure.
Consultations
During a consultation, a hair specialist will review your medical history, explain the procedure in detail, and discuss your expectations. This is an opportunity to ask questions, address concerns, and ensure that you are comfortable moving forward with the treatment.
A professional consultation and treatment performed by a skilled expert will help ensure that your hair removal process is safe and effective.
Conclusion
In conclusion, electrolysis hair removal and laser hair removal are effective methods for achieving long-term hair reduction. Each offers unique benefits depending on your needs and goals. Laser hair removal is quick, efficient, and ideal for larger areas, while electrolysis provides permanent results for those with fine or stubborn hair.
Searching for a dermatologist near me? Dr. Amna at Cleo offers expert advice and tailored care for laser and electrolysis treatments. Get long-lasting, smooth, hair-free skin with safe, effective procedures from a trusted professional.
Looking for electrolysis hair removal cost in Pakistan? Book a consultation for personalized pricing and boost results with expert-recommended skincare products from The Skin Theory.
FAQ’s:
Is electrolysis hair removal permanent?
Yes, electrolysis is the only FDA-approved method for permanent hair removal, as it destroys the hair follicle’s ability to regrow hair.
How much does electrolysis hair removal cost in Pakistan?
Electrolysis treatments in Pakistan typically cost between PKR 2,500 to PKR 8,000 per session, depending on the treatment area and session duration.
Does electrolysis hair removal work on all skin types?
Yes, electrolysis works effectively on all skin types and hair colors, including light, gray, or blonde hair that laser treatments can’t target.
How many electrolysis sessions will I need?
Most people require 10-15 sessions for small areas like the upper lip, while larger areas may need 30-40 sessions spaced 1-2 weeks apart.
Is electrolysis hair removal painful?
Electrolysis causes mild discomfort described as a stinging or tingling sensation, which can be reduced with topical numbing creams.