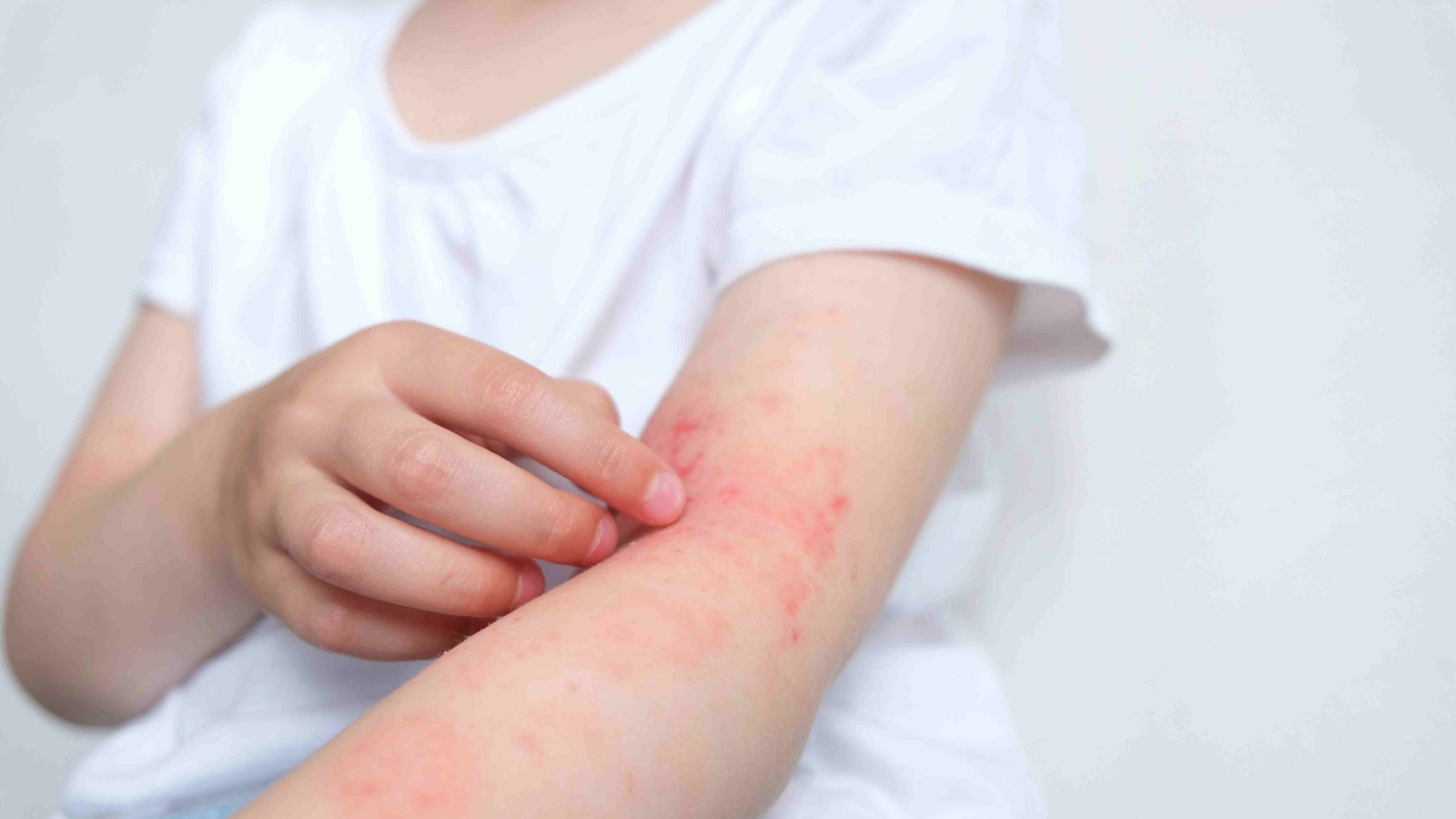
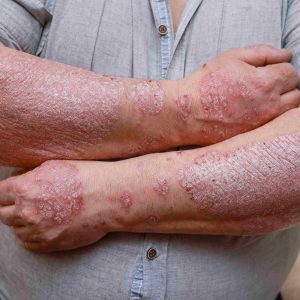
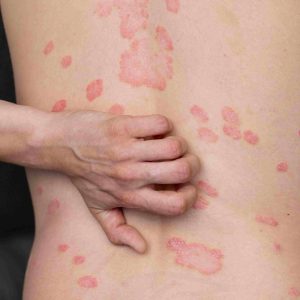
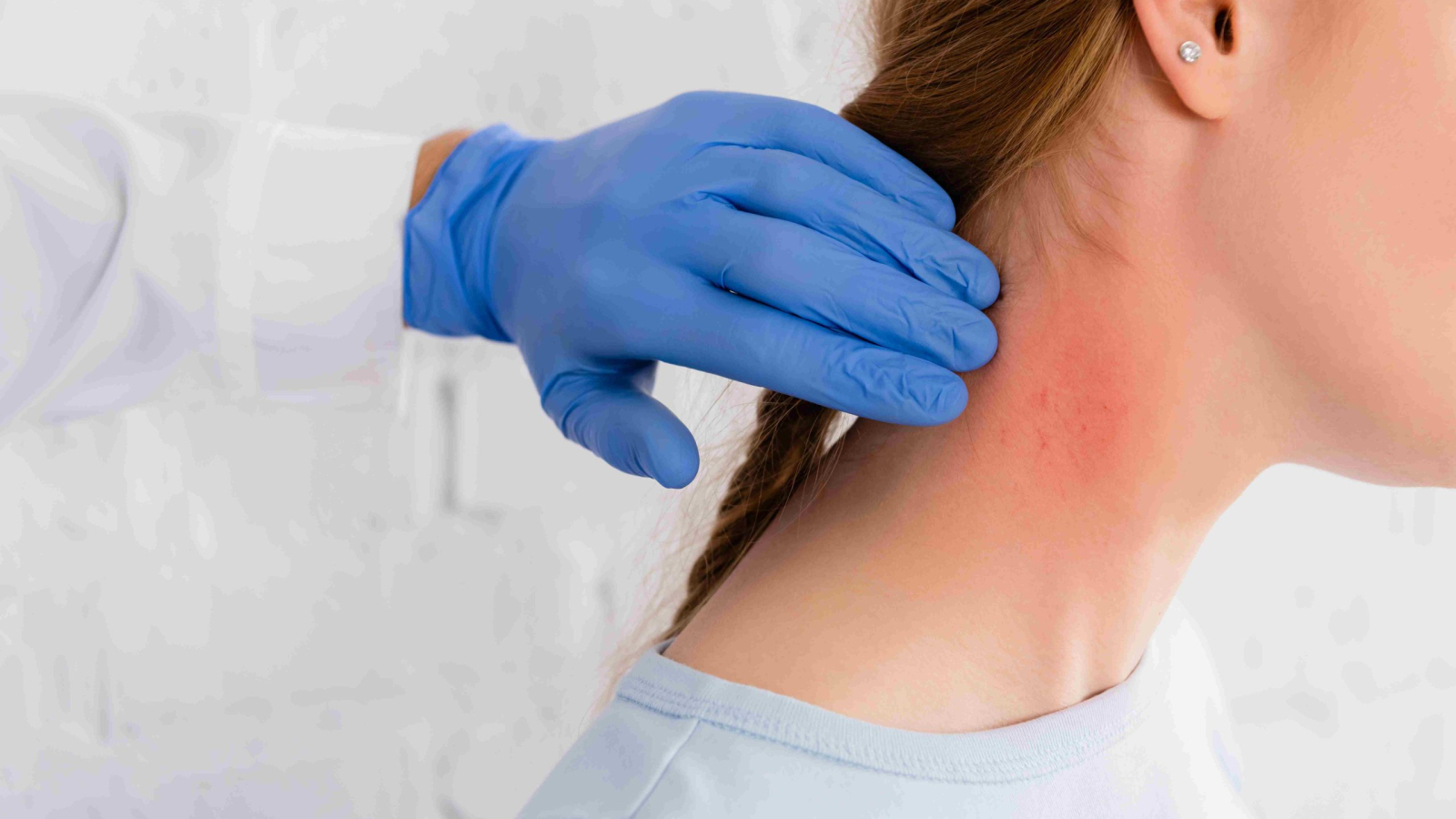
White spots on the skin when they initially show up can be concerning. These patches of hypopigmentation or depigmentation follow from reduced melanin synthesis in specific skin sites.
Usually benign, these varying colour changes might undermine confidence and suggest underlying medical issues. This extensive reference covers the numerous causes of white spots, their symptoms, appropriate treatment options, and when medical assistance is needed.

Typical Reasons for White Patches on Skin
Vitirigo
Affecting over 1-2% of the world’s population in all skin kinds and colours, vitiligo is a persistent autoimmune disorder. Characteristics:- Sharp-edged, completely white patches with total pigment loss
- Symmetrical distribution on both sides of the body in many cases
- Commonly affects the face, hands, armpits, groin, and around the body openings
- May appear suddenly and gradually expand
- It can develop at any age, but typically appears before age 30
- Equal prevalence across genders
- Often has genetic components, with 30% of patients having a family history
- More noticeable on darker skin tones, but equally common across all skin types
Tinea Versicolor (Pityriasis Versicolor)
This common fungal infection affects the skin’s pigmentation and is particularly prevalent in humid, warm climates. Characteristics:- Small, scaly patches that may be lighter or darker than the surrounding skin
- Fine, dust-like scaling on the surface
- Most common on the trunk, shoulders, and upper arms
- May appear slightly pink on light skin or hypopigmented on darker skin
- Often becomes more noticeable after sun exposure
- Most common in adolescents and young adults
- Increases in hot, humid weather
- More common in people who sweat excessively
- It can affect individuals who are immunocompromised

Pityriasis Alba
A common, mild skin condition that primarily affects children and young adults. Characteristics:- Pale pink or red, slightly scaly patches that eventually fade to white
- Round or oval patches typically 0.5-2 cm in diameter
- Primarily affects the face, especially the cheeks, but can appear on the upper arms, neck, and shoulders
- Minimal to no symptoms beyond appearance
- Most common in children aged 3-16
- Often improves or resolves by adulthood
- More visible in darker skin tones or after sun exposure
- Slightly more common in those with atopic conditions
Idiopathic Guttate Hypomelanosis (Sunspots)
These small, porcelain-white spots develop commonly on sun-exposed areas over time. Characteristics:- Round or oval flat spots, typically 2-5 mm in diameter
- Completely white with sharp borders
- Appear primarily on sun-exposed areas: arms, legs, and face
- Asymptomatic with no scaling or textural changes
- More common in fair-skinned individuals
- Prevalence increases with age, especially after 40
- Affects up to 80% of people over age 70
- More common in those with a significant sun exposure history
Milia
These small, white raised bumps are tiny keratin-filled cysts rather than true pigmentation disorders. Characteristics:- Raised, firm, pearl-like bumps 1-2 mm in size
- White or yellowish
- Most common around the eyes, cheeks, nose, and forehead
- Painless and non-inflammatory
- It can appear at any age
- Common in newborns (neonatal milia)
- May develop after skin injuries, blistering disorders, or certain medications
- Can be associated with some genetic conditions
Post-Inflammatory Hypopigmentation
This temporary loss of skin color follows skin inflammation or injury. Characteristics:- White or lighter patches that correspond to sites of previous inflammation
- Irregular shapes reflecting the original injury or inflammation
- May gradually repigment over months to years
- Sometimes accompanied by textural changes
- It can occur at any age
- More common and noticeable in medium to dark skin tones
- Follows any inflammatory skin condition
- Temporary, in most cases, with eventual repigmentation
Treatment Options by Condition
Vitiligo Treatment
Topical Therapies:- Corticosteroids: Medium-to-high potency for limited areas, with monitoring for side effects
- Calcineurin inhibitors (tacrolimus, pimecrolimus): Particularly effective for facial involvement
- Vitamin D analogs (calcipotriene): May stimulate melanocyte activity
- Narrow-band UVB phototherapy: 2-3 sessions weekly for several months
- PUVA (psoralen plus UVA): More aggressive but higher risk of side effects
- Excimer laser: Targeted treatment for smaller areas with higher success rates
- Oral corticosteroids: Short courses for rapidly progressing disease
- JAK inhibitors: Emerging treatments showing promise in clinical trials
- Immunosuppressants: For severe, widespread cases
- Split-thickness grafting
- Suction blister grafting
- Melanocyte transfer
- Punch grafting for small areas
- Monobenzyl ether of hydroquinone permanently removes the remaining pigment
- Creates a uniform appearance when repigmentation is unlikely
Tinea Versicolor Treatment
Topical Antifungals:- Selenium sulfide shampoo (2.5%): Applied to affected areas for 10 minutes daily
- Ketoconazole shampoo or cream: Applied to affected areas for 1-2 weeks
- Clotrimazole, miconazole: Applied twice daily for 2-4 weeks
- Fluconazole: Single weekly dose for 2-4 weeks
- Itraconazole: Short-course therapy
- Ketoconazole: Daily for 5-10 days
- Monthly prophylactic treatment during warm seasons
- Selenium sulfide or ketoconazole shampoo is used once a month
Pityriasis Alba Treatment
Moisturization:- Regular application of emollients to hydrate skin
- Ceramide-containing moisturizers help restore the skin barrier
- Low-potency topical corticosteroids for active, red phases
- Topical calcineurin inhibitors (tacrolimus, pimecrolimus)
- Coal tar preparations for persistent cases
- Daily broad-spectrum sunscreen application
- Proper sun protective clothing
- Avoiding excessive sun exposure, which exacerbates contrast
- Reassurance about the benign nature and eventual resolution
- Patience regarding repigmentation timeline (often 6-12 months)
Idiopathic Guttate Hypomelanosis Management
Cosmetic Approaches:- Sunless tanners to reduce contrast
- Cosmetic camouflage products
- Topical retinoids to stimulate cell turnover
- Mild dermabrasion techniques
- Topical calcineurin inhibitors with limited success
- Cryotherapy for selected lesions
- Comprehensive sun protection to prevent new spots
- Regular use of high-SPF sunscreen
- Protective clothing for sun-exposed areas
Milia Removal
Professional Extraction:- A sterile lancet to create a tiny opening
- Gentle expression of keratin contents
- Quick healing with minimal scarring risk
- Retinoids to increase cell turnover
- Chemical exfoliants (AHAs, BHAs)
- Adapalene or tretinoin for recurrent cases
- Gentle exfoliation
- Avoiding heavy, occlusive skincare products
- Patience, as some milia resolve spontaneously
Post-Inflammatory Hypopigmentation Treatment
Time and Protection:- Natural repigmentation often occurs with time
- Sun protection to prevent worsening contrast
- Patience as melanocytes recover function
- Topical retinoids to stimulate cell turnover
- Low-potency corticosteroids if inflammation persists
- Laser therapy for persistent cases
- Managing primary skin condition (eczema, psoriasis, etc.)
- Preventing future inflammation episodes
- Proper wound care to minimize pigmentation changes
When to Seek Medical Attention
Consult a dermatologist when white patches:- Spread rapidly over short periods
- Develop suddenly without an obvious cause
- Affect sensitive areas (face, genitals, etc.)
- Cause symptoms beyond appearance changes
- Appear alongside other concerning symptoms
- Significantly impact emotional well-being
- Show signs of infection (warmth, increasing redness, pain)
- Fail to improve with over-the-counter treatments